The US has a lack of diversity in its mental health workforce. In 2011, according to the American Psychology Association (APA), psychologists were 85% white, 5% Hispanic, 4% Black, 2% Asian, .28% American Indian or Alaskan Native, and .05% Native Hawaiian or Pacific Islander. Ten years later, in 2021, they were 80% white, 7% Hispanic, 5% Black, 3% Asian, .13% American Indian or Alaskan Native, and .03% Native Hawaiian or Pacific Islander. Very little changed in the span of a decade. There is still a lack of diversity across the mental health workforce, which includes psychiatrists, mental health counselors, and social workers.
Figure 1. Workforce Diversity in Behavioral Health Care
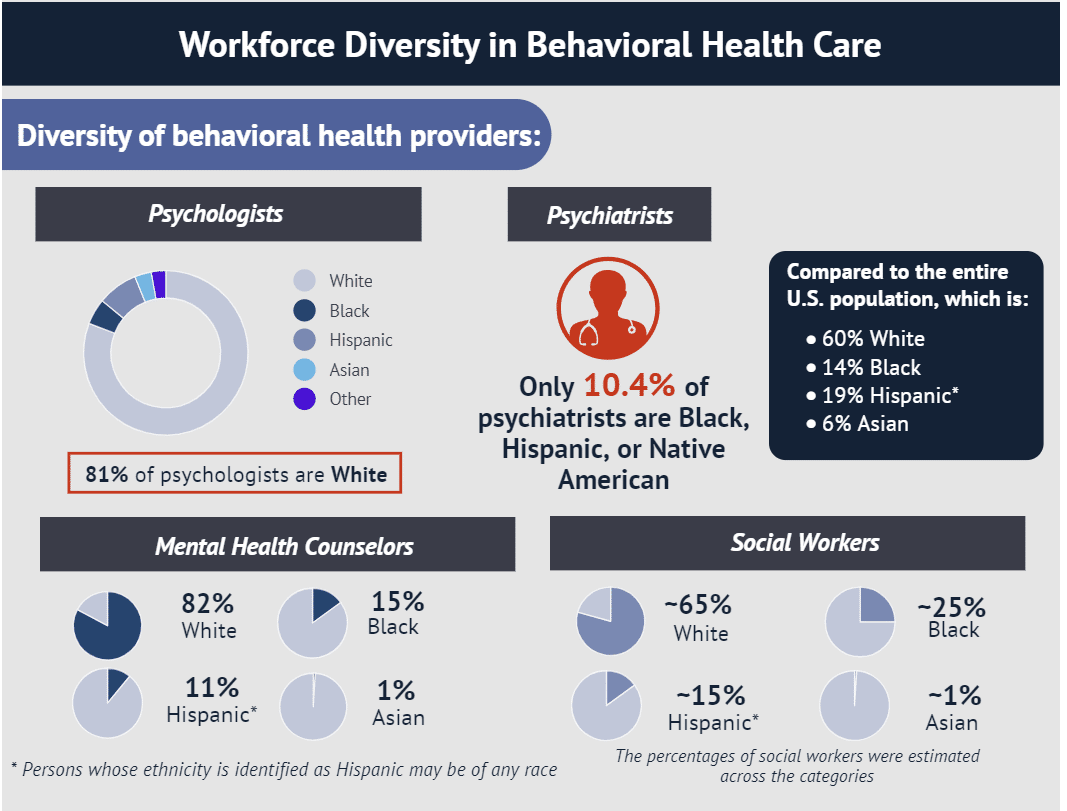
Source: National Institute for Health Care Management Foundation.
This lack of diversity contributes to people of color receiving a lower care quality. A piece by Lyra Health highlights this issue. For example, Black patients tend to be overdiagnosed with schizophrenia and underdiagnosed for bipolar disorder or depression. This is due in part to the fact that “well-meaning therapists may lack a nuanced understanding of their clients’ lived experiences and outlooks.”
People of color and their white counterparts have similar rates of mental health disorders; however, people of color are less likely to receive treatment for their mental health issues. According to the National Institute of Mental Health, in 2020, 52% of white people with a mental illness received treatment but only 37.1% of Black, 35% of Hispanic, and 25.4% of Asian people received treatment. More diverse mental health professionals in the field would help the mental health professional shortage by supplying more providers to help more people, and it would also provide patients of color with better quality care due to greater understanding of lived experiences
There is precedent for this approach. In other areas of medicine diversity has been shown to lead to better outcomes. For example, a 2023 study found evidence that suggests “greater representation of Black PCPs in the PCP workforce is associated with improved survival-related outcomes for Black individuals.”
Why aren’t there more mental health professionals of color in the field?
To increase the number of mental health professionals of color we could use the Jobs to Be Done Theory to understand why there is a lack of diversity. Additionally, it would help uncover the barriers keeping people of color from becoming mental health professionals. Finding out what the barriers are will enable us to address them and increase diversity in the field.
Jobs Theory is a framework that helps us understand individuals’ behavior. It explains that people don’t simply buy products or services (or in this case, simply choose a profession); they “hire” them to make progress in specific circumstances (what we call their Job to Be Done, or “job” for short). Understanding the “job” for which people hire a product or service helps innovators more accurately develop solutions that align with what people are already trying to accomplish.
To uncover the struggling moments, as well as the progress someone seeks in their current situation, an innovator could conduct a Jobs analysis. If you are interested in this process, my colleague, Ann Somers Hogg, wrote about it in a previous blog post.
Here, Jobs is a useful lens to determine the causal drivers behind why people of color want to become mental health professionals and what is keeping them from doing so. It can also uncover why providers of color choose specialties outside of mental health. If health care organizations and medical schools can uncover what is holding people of color back from becoming mental health professionals, it can address those issues or create solutions that alleviate those struggles. The result would be more providers of color in the mental health field, and in turn, there would be a greater likelihood that patients of color receive higher quality care.
Organizations in action
There are already some organizations working to help diversify the mental health field such as Lyra Health, Kaiser Permanente, and the APA. Lyra Health, the mental health provider noted above, is helping increase diversity within the mental health workforce with its fellowship program. Kaiser Permanente is partnering with academic institutions in California that provide degree programs in counseling, social work, or psychology for working professionals through its Mental Health Scholar Academy (MHSA) program. Kaiser employees that attend the partner schools can receive tuition assistance, mentoring, and networking opportunities. MHSA particularly helps support people from ethnically diverse backgrounds seeking to pursue careers in mental health. Additionally, the APA has nine initiatives focused on attracting underrepresented students to the field, including fellowships and student programs.
Diversity matters. And increasing provider diversity within the mental health field can help people of color obtain better mental health services, which could improve their mental and overall health. To achieve these outcomes, we need to know why providers “hire” mental health as a specialty, why they don’t, and what the barriers keeping people of color from becoming mental health professionals are. Then organizations like the APA, Kaiser, and many others can provide programs to help address them.


