If you’re living in the United States, chances are you, or someone close to you, suffers from a chronic disease. According to the CDC, six out of ten adults in the US are diagnosed with at least one, with four out of ten having two or more. The extent of the epidemic is so severe that a whopping 90% of our nation’s healthcare expenditures go toward chronic disease.
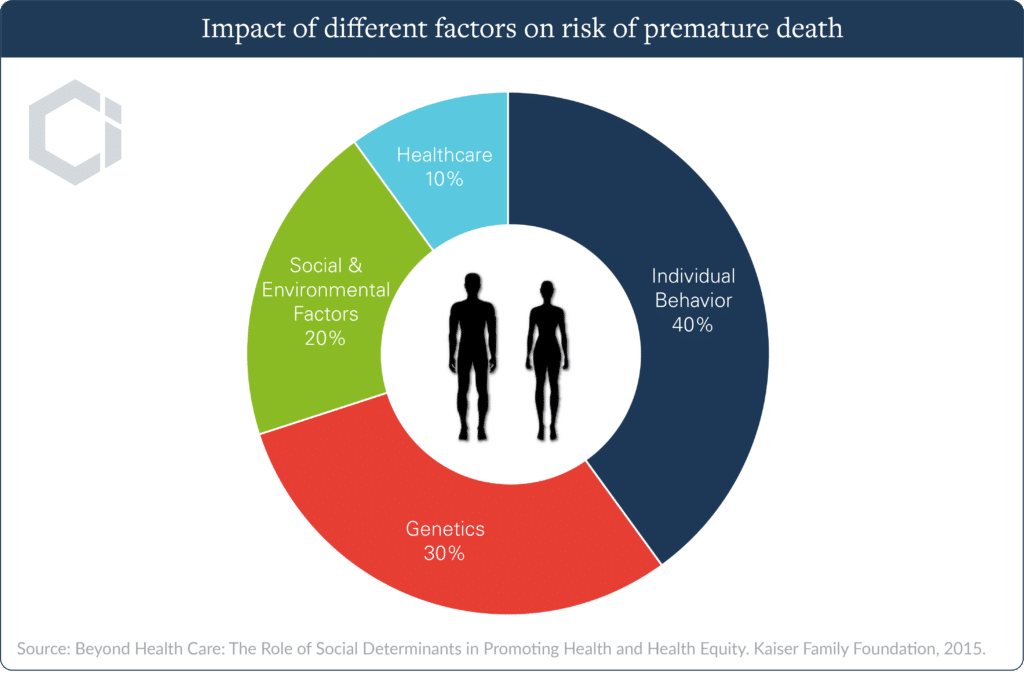
The good news is that many chronic conditions are preventable; diseases like diabetes and heart disease are often caused or exacerbated by unhealthy behaviors such as poor nutrition or a sedentary lifestyle. With individual behavior responsible for 40% of a person’s health status, positive lifestyle changes can go a long way towards reducing the likelihood of chronic disease, and managing their symptoms.
Such lifestyle changes may also make a serious dent in our nation’s healthcare cost crisis too. In 2012, Urban Institute released a study that attempted to quantify their impact. Remarkably, the study found that California spent $362 million dollars that year on chronic diseases that could have been prevented simply through “proven prevention strategies,” such as smoking cessation and changes in diet and exercise. Reducing the prevalence of these chronic diseases by just 1% could save the state of California $3.6 million a year.
That’s a lot of money.
Unfortunately we have yet to see our healthcare system make any meaningful progress in putting preventative care at the forefront of chronic care management. Interventions that could save money and reduce our disease burden, like gym memberships, nutrition coaches, and access to healthy food, are typically far outside of the confines of doctors’ offices and hospitals. Yet many people need help making these healthy lifestyle changes, and would benefit from the support of the healthcare system.
During the second round of Democratic debates just a few weeks ago, more than one candidate acknowledged that the United States has a “sick care” system. Although healthcare professionals are doing everything they can to help people be healthy, the reality is that many providers are overburdened and ill-equipped to tackle these needs. Our current system is designed to treat symptoms rather than prevent disease altogether. As it stands, there is still profit in keeping people sick.
Sky-rocketing pharmaceutical prices are evidence of this broken system, as industry experts and politicians are quick to point out. But pharmaceutical prices are only a small part of a much larger problem. To truly transform our sick care system into a healthcare system, providers must first consider how to better prevent and manage chronic disease to begin with. Fortunately, business models designed to address these challenges are gaining momentum.
What does prevention and management look like?
City Health Works, a Harlem-based organization formed to tackle the chronic disease epidemic, is a promising example of an organization that’s empowering patients to better manage their health and reducing unnecessary spending as a result. The organization was formed as an extension of traditional primary care, providing community-based health coaching for patients with diabetes, hypertension, and asthma in order to create meaningful bonds and teach patients to self-manage their conditions through healthy behaviors.
City Health Works hires coaches directly from the community—which fosters a feeling of trust between patient and coach—and trains new coaches in behavior theory and motivational interviewing. The coaches conduct weekly in-home meetings for three months, and follow up with patients in-person and over the phone for years. Through numerous conversations with patients and their families, coaches help to develop personalized care plans that bridge both clinical and non-clinical needs. Coaches all have medically trained supervisors, who connect with a patient’s primary care provider to update information and address gaps.
Patients see significant improvement in their health, including significant improvement in blood sugar levels. What’s especially impressive is that one out of two patients have an unknown medical issue diagnosed before it reaches a crisis point. Not only has the program improved the health of patients, but in just ten weeks showed an average decrease of $600 in spending per member per month.
We could do a lot of things with $362 million; work to alleviate hunger and homelessness, invest in education, etc. If just one state could save that much money by focusing on prevention instead of treatment, what could the country as a whole do?


