Health care has a long and storied history in the United States, and much has been said about its failings: it’s too expensive, our health outcomes are poor, our life expectancy is lower than that of other high-income countries, et cetera. Late Harvard Business School professor, Clayton Christensen, even said in his 2009 Mayo Transform presentation, “a general hospital actually is not a viable business model. In the absence of philanthropy, subsidy, and heavy regulation, most would collapse under their own weight.”
Most would agree that we have plenty of opportunities for improvement within our national health care ecosystem. Yet one area where there seems to be disagreement is around how to refer to this ecosystem.
Is it “health care” or “healthcare”?
Some will conclude that it doesn’t matter. But here I’ll lay out why it does: language is a powerful tool to both ignite and embody progress.
We’ve seen language serve these purposes across industries in our nation. Dunkin’ Donuts became just Dunkin’. Weight Watchers is now WW. Stewardesses are now flight attendants, in support of women’s rights in the workplace. We shifted our language from homeless to houseless to represent class inclusivity, and the list continues.
In light of language’s ability to transform mindsets, we believe “health care” is preferred over “healthcare” for three reasons. Let’s dig into what those are.
1. Health care capitalizes on logic
The health care industry is made up of multiple facets and subspecialties. Behavioral health or mental health, women’s health, cancer care, cardiac care, musculoskeletal care, primary care, various digital health offerings, and many more. However, “healthcare” is the only industry-defining term where two words are combined into one. This inconsistency is illogical, and as a result, “health care” is a more efficient way to frame the topic at hand.
2. Health care connotes serving the consumer
By calling it “healthcare,” industry insiders insinuate that the words are more about what they reactively provide once illness or a chronic condition has already taken root, versus proactive solutions aimed at serving people’s needs.
Therefore, continuing to use the term “healthcare” perpetuates a key issue inherent in the industry’s outlook. The industry is historically supply-oriented in its approach to business. This means that its business model is organized around its capabilities, especially its resources, instead of being organized around the value proposition it offers consumers and customers.
In the diagram below, you’ll see a juxtaposition of the traditional, fee-for-service, sick care business model on the left—which represents a supply-orientation—versus one effectively addressing the drivers of health (DOH) on the right. The diagram on the right represents a business model that is consumer- and customer-centric, or demand-side oriented.
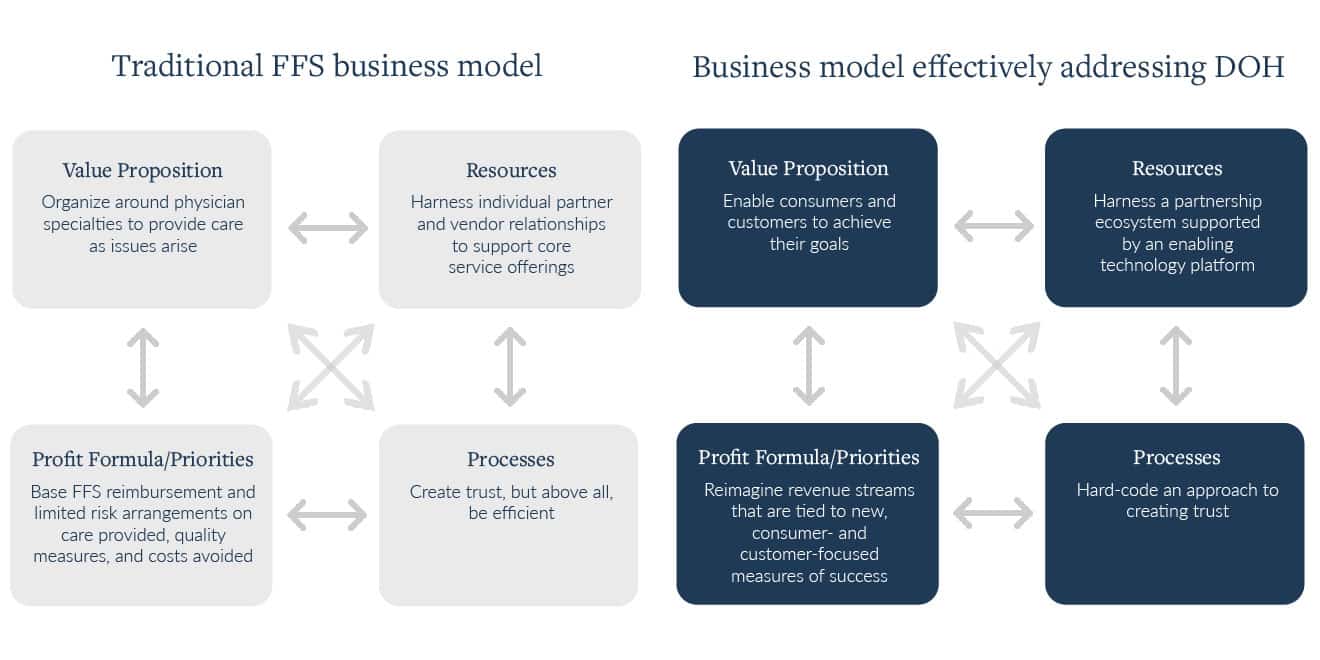
The “rebranding” of the industry from one that focuses on sick care to improving health isn’t just paying lip service to a trend. Speaking to the necessity of demand-orientation, Todd Dunn, VP of Innovation at Atrium Health, recently stated in a Digital Patient podcast, “Success is a race to some degree. Everyone is…racing to win the customer or consumer. And if you embrace the status quo, somebody else isn’t, and you’ve accepted your fate.” For incumbents to not only maintain cultural relevance, but, quite bluntly, ensure their business model viability into the future, it’s time to make a mindset shift with the help of the associated language shift that accompanies it.
3. Health care better (not perfectly) encapsulates the progress people seek in their struggling moments
The industry must accept that people seek out care in order to live their lives, and better health is a means to an end. In performing hundreds of user interviews while working for a health system, I didn’t encounter anyone who desired to receive more “healthcare.” They sought more of their lives and saw “health” as a way to live the life they desired, and “care” as a step on the pathway to achieve that health.
In their minds, health and care were not one thing. They were two separate, but related factors. This is an example of what’s called a Job to Be Done. That is, a person seeks care to resolve a struggle they’re facing in their lives. As I’ve written about before, health care’s various offerings get “hired” by different people under different circumstances when a struggling moment arises in their lives, and they have a specific type of progress they are seeking.
For example, if a woman is seeking to deliver a healthy baby, she may hire an OBGYN and the hospital where that provider delivers to help her achieve that progress. She may also hire a midwife and the option to give birth at home. The latter option would traditionally be seen as occurring outside of the health care system. But is it? It’s care provided by a health professional that helps someone achieve more of the progress they seek in their lives.
Employing a demand-side perspective and using language that better encapsulates the progress people seek helps organizations better serve their customers and consumers, and thus enhance their competitiveness in the marketplace. But those who choose to look inward, focusing on the services they offer, will find a shrinking pool of patients seeking to be served at their doors.
So, while “health care” as two words may get a future update to better embody the end user’s perspective and further address the industry’s supply-side outlook, it’s certainly better than using “healthcare” for the time being. And that’s because it can serve as a transformative aid to ignite, and ultimately embody, progress.


