It’s that time again: the 2020 Election is fast approaching, and candidates are lining up to be the potential 46th President of the United States.
On June 26 and 27, 20 Democratic candidates took the stage in the first primary debate of the election season. Given that the US spends more money per capita on healthcare than any other country—and yet boasts some of the worst results including a higher rate of medical errors and a higher disease burden—much of the discussion unsurprisingly surrounded the topic of healthcare. There was an understandable sense of urgency around fixing a healthcare system that is not working for many patients, employers, or medical professionals, making healthcare one of the critical policy issues of our time.
While the refrain of “healthcare is a right” echoed from all of the debating candidates, the approaches to ensuring that right differed widely. That’s because transforming our broken system is no simple matter, as countless presidents have learned from first-hand experience.
So how do we get healthcare right? Regardless of who leads in the polls, here are the topics that anyone looking to revamp the healthcare system in the US should consider.
1. A broader focus on the Social Determinants of Health
Social and environmental factors, like education and infrastructure, have at least twice the impact on the risk of premature death than medical care. During the debates, Cory Booker was the only candidate that demonstrated an understanding of the complex relationship between health and other fields, observing that the lack of access and coverage is more than a healthcare problem, but also an education, employment, and retirement problem. For example, the level of education one has plays a role into how healthy a person is, and subsequently how healthy a person is impacts the education level one is able to attain. Thus social and environmental factors not only influence one’s healthcare but also result from one’s healthcare.
Those looking to design a better healthcare system can improve healthcare outcomes by addressing these links. We’ve seen promising results from innovative primary care providers, such as Iora and Oak Street, which are improving outcomes for patients by providing resources for healthier food, and offering health literacy classes, among other socially driven initiatives. Following their lead, policymakers must not only acknowledge the social and environmental factors that impact our health but design with them in mind.
2. Stronger attention on chronic illness
Chronic illness accounts for 86% of all US healthcare spending and afflicts 60% of American adults. Any effort to reduce healthcare spending needs to take into account how we approach the epidemic and care for the afflicted. This goes well beyond the debate surrounding prescription drug costs.
In our current system, it is—frankly—more profitable to treat people rather than cure them. Marianne Williamson rightly called the current healthcare system a “sick care” system, where providers simply treat symptoms as they arise. In looking to improve care for chronic illness, providers and innovators need to search for holistic health solutions that help patients reach their goals, realizing that patients are more likely to engage in healthy behavior when it aligns with the progress they’re already trying to make. Better yet, these solutions need to be based in a business model that rewards curing patients, rather than treating them.
3. Reimbursement based on outcomes, not services
Thus far in the presidential campaign, most of the buzz around healthcare comes in the form of the “Medicare for All” debate—whether or not the US should forego private insurance in favor of a federally-run health coverage plan. However, while candidates are focused on the question of who will facilitate health insurance, they are missing the far more important issues of how health payments will be structured.
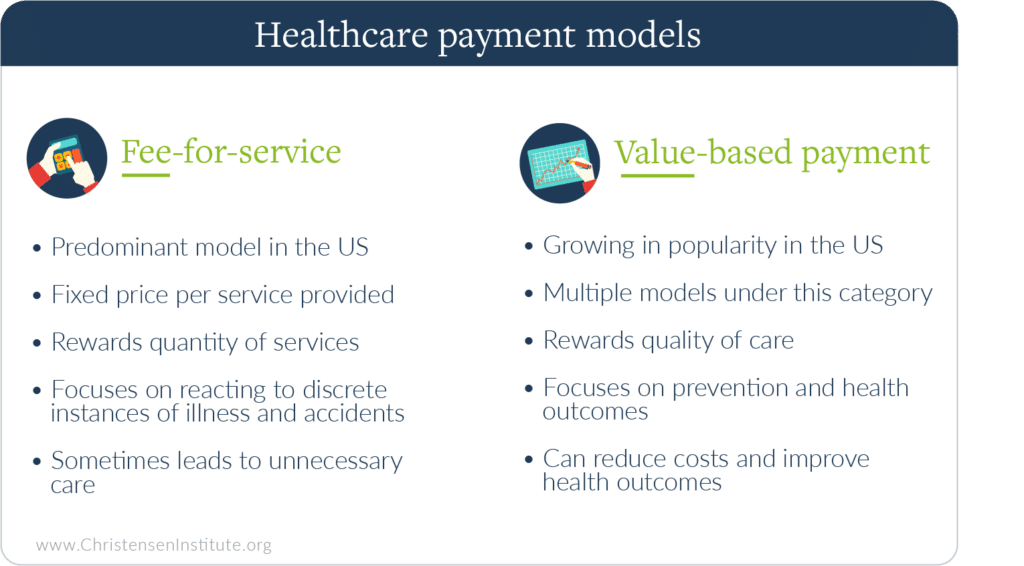
The predominant healthcare business model in the US does not currently reflect the goals and changes that need to be made in our healthcare system. Much of the current healthcare system rewards providers and payers for every service they provide, not on the quality of the care provided. If the US is to change the priorities of our healthcare system—-from one that focuses on dispensing care to one that focuses on maximizing health—then it needs to be paired with payment models that reward wellness and improved outcomes. This is the goal of integrated payer/provider systems, such as Kaiser, Geisinger, and Intermountain, where incentives are aligned to reward providers for keeping patients healthy. Whether private insurance ceases to exist or not, the fee-for-service model cannot exist as it stands if the goal is to improve healthcare outcomes.
2020 hopeful Pete Buttigieg summed up the need for change in healthcare nicely, stating “…our country is healthier when everybody is healthier.” In order for policymakers to work towards this goal we need to identify and understand what’s keeping people from being healthy in the first place. Policies that recognize that health goes beyond just medical care, and help our nation transition away from a “sick” care system, will go far in making the US a healthier country.


