This guest blog was written by Dr. Vikram Devalia, a practicing clinician from the United Kingdom with a special interest in applying business theory to improve healthcare systems.
Over the past twenty years, innovators, policymakers, and administrators have worked tirelessly to reimagine the U.S. healthcare system in order to better serve the needs of the public. Yet transformative change has largely proven elusive. In such a fragmented industry, a unique set of management tools are required to launch an initiative that breaks the mould and realigns the system with the shifting health demands of the public. Although seemingly an impossible task, this feat was achieved just 70 years ago by one Aneurin Bevan.
The National Health Service: Flawed but treasured
2018 marks the 70th birthday of the founding of the United Kingdom’s National Health Service (NHS). The NHS is a universal coverage system funded 98% through general taxation contributions. For the past 70 years, British citizens have enjoyed care free at the point of access, based on clinical need rather than ability to pay.
This somewhat idyllic system, however, is not without its fair share of problems. Dated healthcare delivery models, an aging population and a lack of investment resulted in the “humanitarian crisis” of Winter 2015, as labelled by the British Red Cross charity who stepped in to support struggling frontline emergency services. Furthermore, waiting times for specialist treatment and elective operation cancellation rates continue to increase year on year. Nevertheless, public support and faith in the NHS remains resolute. Why? Appreciating the context of the NHS’s foundation is helpful for understanding this phenomenon.
The NHS was founded in 1948, emerging at a time when World War II had torn the country apart but brought a community together. Many inequalities in society had been highlighted and formed the backdrop for the NHS’ founding principles. As a consequence, the NHS represents more than just a provider of healthcare. It is the symbol of a paradigm shift in the socio-political context of a nation. Despite its almost cult-like status in Britain today, its founding father Aneurin Bevan faced a whole different set of circumstances when he first proposed his plans for a universal coverage system.
Bevan came from humble beginnings. As one of ten siblings born into a poor coal miner’s family in the South Wales Valleys, he appreciated from an early stage the importance of widening access to healthcare for a more ‘wholesome’ society. His early experience of politics at his local trade union, the South Wales Miner’s Federation, and healthcare systems, whilst serving on the Hospitals Committee of the Society, provided the inspiration for his quest toward creating a nationalised healthcare system. Bevan was elected minister for health in 1945 and by 1948 the NHS was already treating its first patients. Applying the Theory of Tools of Cooperation and Change, it becomes clear how Bevan was able to achieve such a feat in such a short amount of time.
The Theory of Tools of Cooperation and Change
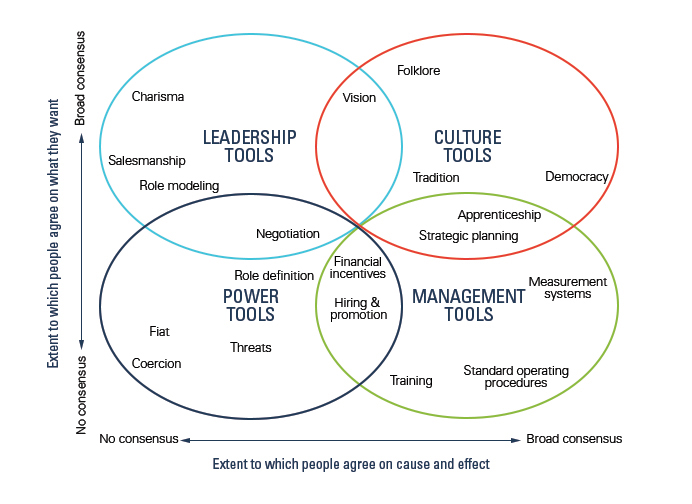
In 2006, Christensen et al. proposed a framework to help managers understand their environment and adopt the best approach to be able to effect meaningful change. The framework requires, first, an assessment of all relevant stakeholders across two critical dimensions: (1) the extent to which they agree on a goal and (2) the extent to which they agree on how to achieve that goal. Plotting these dimensions on a 2×2 ‘agreement matrix’ helps managers to narrow down which category of management tools are best suited to a particular situation. While the parameters are not meant to be rigid, the Tools of Cooperation and Change are categorized into four types—power tools, leadership tools, culture tools, and management tools—and can range from heavy-handed coercion to influential storytelling.
Of course, Bevan was unaware of such theory, but by virtue of his innate ability, he was able to deliberately analyse the environment deploy the right management tools to make his vision a reality.
Figure 1: Tools of Cooperation and Change Agreement Matrix
Applying the theory to mobilize stakeholders
On initially revealing his plans for a taxpayer funded universal coverage system, Bevan encountered a mixed response. He had the support of an adoring working class populace but faced furious opposition from many other key stakeholders including Doctors’ Unions, the opposing political party and even colleagues within his own cabinet.
The working classes had always favoured the principles of free healthcare set out in Bevan’s plans but needed a leader with the ability to formulate a feasible plan, and the authority to translate this into reality. As health minister, Bevan was able to fulfill this role by using leadership tools to rally support from those who were likeminded. He used his prior political and healthcare-specific experience to draw up proposals for a new healthcare strategy and provided a voice for the people in parliament. Throughout his tenure, Bevan also used his charismatic and engaging personality to strengthen wider public support for his vision for free healthcare for all.
Bevan also realised that he had to adopt a different approach with those whose goals weren’t aligned with his. For these groups, Bevan deployed power and management tools. He used strong financial incentives for doctors concerned about the implications of a state-run system on their wages, including allowing primary care physicians to continue practicing as independent businesses. Unable to use money to convince politicians, Bevan placed sustained pressure on members of his own cabinet who resisted his plans by leveraging the growing public support, forcing them to rethink their stance. With politicians of the opposing political party, he persevered years of tough negotiations. Eventually his efforts bore fruit, and on July 5th, 1948 his dream became a reality with 13-year-old Sylvia Diggory becoming the first patient to be treated by the NHS.
Bevan’s management of the different stakeholders is a powerful example of how deploying the correct tools in a given situation can create the right environment for a whole industry to change. Within just three years, he was able to accomplish the inconceivable and change the landscape of healthcare delivery for a nation forever. Regardless of one’s political perspective, Bevan’s achievement cannot be refuted. Given the problems faced in healthcare on both sides of the Atlantic, perhaps healthcare leaders can learn from Bevan and apply the Tools of Cooperation and Change to initiate the changes within their systems that are so desperately needed.